Understanding Ultrasound and Sonogram: Modern Medical Imaging Explained
Most people’s only experience with ultrasound is a grainy prenatal photo taped to a fridge. Fair enough. But limiting your understanding of this technology to baby pictures is a bit like thinking of a stethoscope as the thing your doctor wears around their neck for decoration. Ultrasound is one of the most useful diagnostic tools in medicine, and it’s changing faster right now than at any point in its sixty-year history.
If you’ve ever wondered what the difference between an “ultrasound” and a “sonogram” is, whether your family doctor can actually do one in the office, or what it means that artificial intelligence is starting to read these images alongside clinicians, keep going. This stuff matters more than most people realize.
The Terminology People Always Mix Up
An ultrasound is the procedure. A sonogram is the image it produces. That’s it. The distinction is roughly the same as saying “photograph” versus “camera.” One is the tool doing the work, the other is what comes out of it. Nobody will correct you at a dinner party if you swap them, and your doctor won’t blink either. But if you want to be precise, an ultrasound machine sends high-frequency sound waves into your body, those waves bounce off your organs and tissues at different speeds depending on tissue density, and the returning echoes get translated into a visual image. That image is the sonogram. In practice, clinicians use both words interchangeably and everyone understands what’s meant. The technology is the interesting part.
What’s Happening Inside the Machine
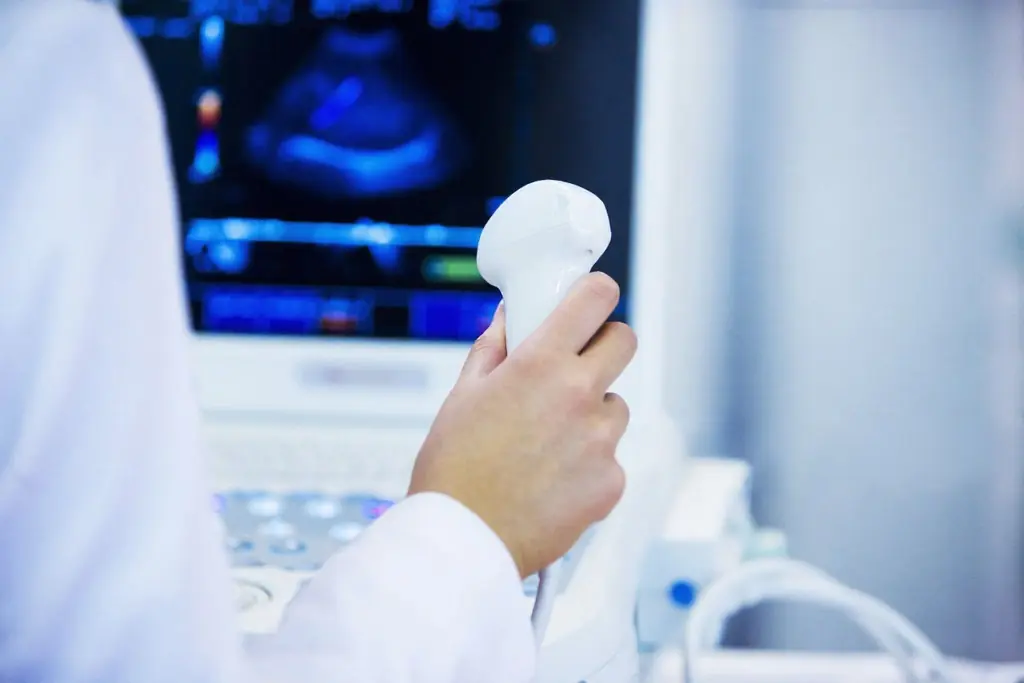
Ultrasound machines operate at frequencies between 2 and 18 megahertz, well above the range of human hearing (we top out around 20 kilohertz). The physics are elegantly simple. The machine’s transducer sends a pulse of sound into your body. When that pulse hits a boundary between two different tissue types, say the edge of your liver against surrounding fat, part of the sound bounces back. The machine measures how long the echo took to return and how strong it was, then uses those two data points to build an image, pixel by pixel. Lower-frequency probes penetrate deeper into the body but produce less detailed images, which makes them useful for abdominal organs. Higher-frequency probes sacrifice depth for resolution, making them better for superficial structures like tendons and thyroid glands. A skilled sonographer chooses the right probe and adjusts settings in real time, which is part of why ultrasound interpretation is more operator-dependent than, say, a CT scan. The quality of what you see depends heavily on who’s holding the probe.
Why Your Family Doctor Might Soon Have One in Their Pocket
The single biggest shift in ultrasound over the past decade is miniaturization. Point-of-care ultrasound, usually called POCUS, has put something that used to require a rolling cart and a hospital department into a device the size of an electric razor. These handheld probes connect wirelessly to a tablet or smartphone. They cost between $2,000 and $8,000, a fraction of traditional hospital-grade machines that run $100,000 or more.
For family medicine, this changes the calculus on when and where imaging happens. A patient walks in with right upper quadrant pain. Before POCUS, that visit ends with a requisition for an abdominal ultrasound at an imaging center, a wait of days to weeks for the appointment, and then more days for the report to come back. With a handheld probe, the doctor can check for gallstones in the exam room in under five minutes. Someone presents short of breath and you’re worried about fluid around the lungs? You can visualize it immediately and decide whether to send them to the ER or manage it outpatient.
The evidence backing POCUS in primary care is growing steadily. A 2023 systematic review in the Annals of Family Medicine found that POCUS improved diagnostic accuracy in primary care settings across multiple clinical scenarios, from musculoskeletal complaints to abdominal pathology. The Canadian Medical Association has increasingly endorsed POCUS training as part of residency programs, and provincial medical associations are working through the billing and credentialing frameworks to make office-based ultrasound sustainable for family physicians. We’re still in the early adoption phase, but the trajectory is clear: within a decade, a probe in the office will be as standard as the blood pressure cuff.
AI Isn’t Replacing Sonographers, But It’s Making Them Better
Artificial intelligence in medical imaging gets a lot of hype, most of it overblown. But in ultrasound specifically, AI is solving a real problem. Unlike CT or MRI, where the machine produces a standardized set of images regardless of who operates it, ultrasound quality varies enormously with operator skill. The image you get depends on probe positioning, pressure, angle, and a dozen other subtle physical adjustments. This makes ultrasound simultaneously one of the most accessible and most operator-dependent imaging modalities.
AI algorithms are addressing this gap from two directions. First, real-time guidance: newer systems can coach less experienced operators on probe placement, essentially telling them “tilt left, press harder, you’re looking at the wrong plane.” Second, automated image interpretation: once you have an image, AI can flag potential abnormalities, measure structures, and identify patterns that a human eye might miss when scrolling through hundreds of frames. A 2024 study in Nature Medicine demonstrated that an AI system reading cardiac ultrasounds matched or exceeded the diagnostic accuracy of board-certified cardiologists for detecting reduced ejection fraction, a key marker of heart failure. The system processed studies in seconds versus the minutes required for human interpretation.
This doesn’t mean AI is about to replace the radiologist who reads your ultrasound report. Ultrasound interpretation requires clinical context that algorithms don’t have access to. What it means is that a family doctor with basic ultrasound training, assisted by AI guidance software, can now perform screening-level assessments that previously required specialized expertise. For a healthcare system where wait times for diagnostic imaging run weeks to months, that’s a meaningful capacity expansion.
Elastography: Squeezing More Information From Sound
One of the more interesting recent additions to the ultrasound toolkit is elastography. Standard ultrasound tells you what structures look like. Elastography tells you how stiff they are. This matters because many disease processes change tissue stiffness before they change tissue appearance. Liver fibrosis, which progresses toward cirrhosis, makes liver tissue progressively stiffer. Malignant tumors tend to be harder than benign ones. Inflamed tendons lose their normal elasticity.
In liver disease, elastography has been particularly consequential. Before it became widely available, the standard method for assessing liver fibrosis was a biopsy: a needle inserted between the ribs to extract a tissue sample. Biopsies carry a small but real risk of bleeding and are uncomfortable enough that patients often delay or avoid them. Elastography provides a non-invasive alternative that correlates well with biopsy findings for detecting significant fibrosis. European and North American hepatology guidelines now recommend elastography as a first-line screening tool for patients with chronic liver disease, effectively replacing biopsy as the initial assessment in many clinical scenarios. For breast imaging, elastography adds a layer of information that can help distinguish suspicious masses from benign ones, potentially reducing unnecessary biopsies. The same principle applies to thyroid nodules, where stiffness measurements help stratify which nodules need further workup and which can be monitored safely.
What Ultrasound Sees Well, and Where It Falls Short
Sound waves travel beautifully through fluid and soft tissue. They bounce usefully off organ borders, vessel walls, and tumors. Ultrasound is excellent for the liver, gallbladder, kidneys, bladder, uterus, ovaries, thyroid, heart, blood vessels, muscles, tendons, and joints. It can detect gallstones, kidney stones, blood clots in leg veins, aortic aneurysms, pericardial effusions, tendon tears, and joint fluid collections, all without radiation and usually without any preparation beyond showing up.
But sound waves bounce off bone and scatter in air, which creates two major blind spots. Anything behind bone, like the brain in adults, is essentially invisible to ultrasound (neonatal skulls are thin enough that brain ultrasound works in infants, but that window closes). Air-filled structures like lungs and intestines are difficult to image in detail, which is why CT remains the workhorse for pulmonary and bowel pathology. These aren’t limitations that technology will overcome, because they’re fundamental to the physics of how sound interacts with matter. Knowing what ultrasound can’t do is just as important as knowing what it can.
The other limitation worth mentioning is body habitus. Ultrasound waves attenuate as they pass through tissue, and more tissue means more attenuation. In patients with a higher BMI, image quality drops, particularly for deep abdominal structures. This is a clinical reality that doesn’t get discussed enough, and it sometimes means that an ultrasound that would be diagnostic in a thin patient yields inconclusive images in a larger patient, requiring follow-up with CT or MRI.
What It’s Like to Get One Done
If you’ve never had a non-prenatal ultrasound, the experience is straightforward. A sonographer applies warm gel to your skin over the area being examined. The gel eliminates the air gap between the probe and your skin, because remember, air is the enemy of sound wave transmission. The sonographer presses the probe against your skin and moves it around, sometimes asking you to hold your breath, roll to one side, or change position so they can get views from different angles. The whole thing takes fifteen to forty-five minutes depending on what’s being examined, and it doesn’t hurt, though the probe pressure can be uncomfortable if the area being examined is already tender.
For an abdominal ultrasound, you’ll typically need to fast for eight to twelve hours beforehand, because food stimulates gallbladder contraction and bowel gas, both of which degrade image quality. Pelvic ultrasounds often require a full bladder, which provides an acoustic window to see the uterus and ovaries more clearly. For most other types, including musculoskeletal, vascular, and thyroid, no preparation is needed.
After the exam, a radiologist reviews the images and generates a report that goes to your ordering physician. The turnaround time varies from same-day at some facilities to a week or more at busy hospital departments. Your doctor reviews the report and discusses the findings with you. If the images were inconclusive or showed something unexpected, further imaging or referral may follow.
Where This Is All Heading
The convergence of miniaturization, AI, and expanding clinical applications is pushing ultrasound into a new role in healthcare delivery. It’s becoming less of a specialist tool you get referred for and more of a primary care instrument used at the point of first contact. The evidence supports this shift. A 2023 meta-analysis in BMC Primary Care found that POCUS changed clinical management in 25% to 70% of primary care encounters where it was used, most often by confirming a suspected diagnosis or ruling out a dangerous condition without the delay of a formal imaging referral.
Contrast-enhanced ultrasound, which involves injecting microbubble contrast agents intravenously, is expanding what can be visualized. It’s particularly useful for characterizing liver lesions and assessing tissue perfusion. Therapeutic applications are emerging too: focused ultrasound can deliver targeted heat energy to destroy uterine fibroids or, in combination with microbubbles, temporarily open the blood-brain barrier to allow drug delivery to the central nervous system. These applications are still largely in specialized centers and clinical trials, but they represent a genuine expansion of what sound waves can accomplish in medicine.
For patients in Canada’s system, where diagnostic wait times are measured in weeks and months rather than days, the expansion of office-based ultrasound into primary care could meaningfully reduce the time between symptom onset and diagnosis. That gap is where anxiety lives, where conditions progress, and where preventive intervention works best. Anything that shrinks it matters.
If you have questions about imaging, diagnostic testing, or what screening might be appropriate for your situation, that’s a conversation worth having with your family doctor. If you don’t have one, that’s a problem worth solving first. Read our guide on how to navigate the Canadian healthcare system, or if you’re in downtown Toronto, Button Health is a new Family Health Organization opening summer 2026 at 790 Bay St. #536 in the Bay St. Corridor. Visits will be covered by OHIP. Join the priority list for first access to book when we open.
Join our patient waitlist here.
Have questions about ultrasound or other medical imaging? Talk to us about which tests might be right for you.